In this article, you will learn about the different atrial dysrhythmias, including premature atrial complexes (PACs), atrial flutter, atrial fibrillation and supraventricular tachycardia. The EKG Interpretation video series follows along with our EKG Interpretation Flashcards, which are intended to help RN and PN nursing students study for nursing school exams, including the ATI, HESI, and NCLEX.
EKG Interpretation - Nursing Flashcards
Atrial rhythms
The key characteristics of atrial rhythms are abnormal P waves, or P waves that are replaced by flutter or fibrillation waves. Remember from our overview on EKG basics that the expected duration of a P wave is .06-.12 seconds, and the expected amplitude (height) is 2.5mm or 2.5 small boxes.

Premature atrial complexes (PACs)
Premature atrial complexes (PACs) are a common kind of heart dysrhythmia characterized by premature electrical impulses originating from the atria and occurring too early.
Premature atrial complexes on an EKG
When observing a PAC on an EKG, you will notice that the P wave will appear prematurely. It will have a different look than other P waves, and it may be hidden in the preceding T wave.
Depending on the prematurity of the impulse, PACs can also affect the QRS complex on an EKG. There could be a long pause following the QRS complex, it could cause an abnormally wide QRS complex and can even cause the QRS complex to drop off the EKG completely.
Treatment of PACs
Treatment of PACs is not usually necessary, however, frequent PACs may precede more serious dysrhythmias and they should be monitored closely.

Atrial flutter
Atrial flutter is a type of heart dysrhythmia that occurs when the upper heart chambers (atria) beat faster than the bottom chambers (ventricles).
Atrial flutter on an EKG
When observing atrial flutter on an EKG, the first thing you will notice is that there appear to be multiple sawtooth-like P-waves for every QRS complexes. This means that the atria are beating at a rate 3-4 times the ventricular rate, which is much too fast. Although they may look like P-waves, in atrial flutter these are actually called "flutter waves," or F-waves.
The QRS complexes on an atrial flutter strip will usually be normal and will be under 0.12 seconds in duration.
With atrial flutter, the heart rate will be very, very fast and will be between 250 and 400 beats per minute.
Treatment for atrial flutter
Treatment for atrial flutter can include the use of antiarrhythmic drugs, specifically calcium channel blockers like verapamil and diltiazem. Another treatment option is cardioversion, which is a procedure that restores the heart's normal rhythm by sending electric shocks via electrodes placed on the chest.
Verapamil and diltiazem are two key medications to know for your Pharmacology class, and they are covered in our Pharmacology Flashcards!
Atrial fibrillation (Afib)
Atrial fibrillation is a dysrhythmia that can lead to blood clots, stroke, heart failure and more. With atrial fibrillation, the upper chambers of the heart the atria beat very irregularly.
Atrial fibrillation on an EKG
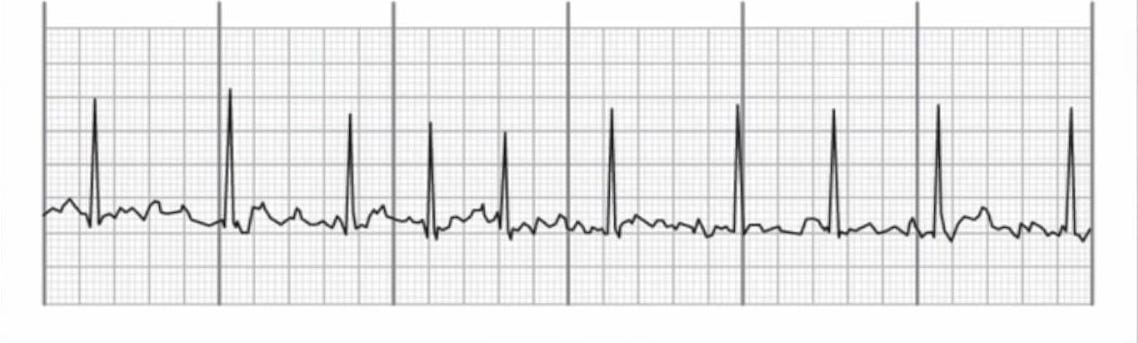
When observing atrial fibrillation on an EKG, the first thing you will notice is that instead of P waves before the QRS complex, there will be lots of little bumps or "fib waves" between QRS complexes.
Distances between R waves will be irregular and the distance between fib waves will vary.
QRS complexes are typically normal in duration at under 0.12 seconds.
The atrial rate for someone with afib will be very fast at between 350 to 600 beats per minute. You will not be able to measure it with your calipers using any box method. You will count the ventricular rate by counting the number of QRS complexes.
Treatment of atrial fibrillation
Patients with afib can be treated with cardioversion as well as antiarrhythmics. Patients with afib are also at high risk for blood clots, stroke and pulmonary embolisms. It is very important that patients receive anticoagulation (blood thinner) medication like warfarin. in order to prevent a blood clot from forming, traveling to the brain, and causing a stroke or thromboembolism.

Supraventricular tachycardia (SVT)
Supraventricular tachycardia (SVT) describes an abnormally fast heart rate that originates above the ventricles, typically in the atria. "Supra" means above, and ventricular means ventricles, so supraventricular literally means "above the ventricles." Even though ventricular is in the name of this rhythm, it is not a ventricular rhythm, which is a very common mistake.
SVT is considered an umbrella term and includes sinus tachycardia, paroxysmal supraventricular tachycardia, as well as atrial fibrillation and atrial flutter, which we already covered.
Why is sinus tachycardia included in this umbrella if it's a sinus rhythm? Supraventricular tachycardia can actually occur between stretches of normal sinus rhythm.
SVT on an EKG
When observing an SVT on an EKG, the distance between R waves will be equal and pretty regular.
The heart rate for a patient with SVT will be over 100 beats per minute, typically between 150 and 250 beats per minute.
Unfortunately, because the heart rate is so fast, it's hard to evaluate the atrial heart rhythm.
P waves are typically not visible, or if they are, they will be buried in the T wave, making it very difficult to evaluate correctly.
With SVT, the QRS complex will be normal. It will be narrow and under 0.12 seconds in duration.
Treatment for SVT
For treatment of patients with SVT, we can use cardioversion or treat the patient with antiarrhythmics. There is a very special drug to treat SVT, which is not used for any other cardiac arrhythmia: adenosine. This drug is also covered in our Pharmacology Flashcards!



1 comment
Wao! Amazing explanation!